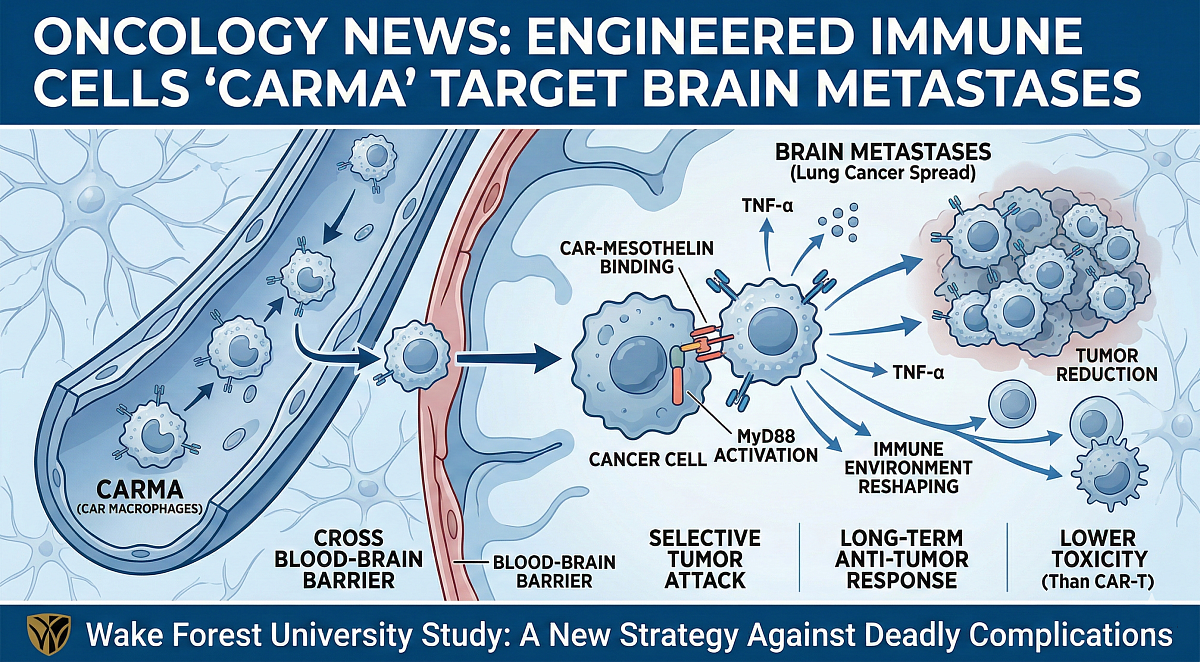
A new study by researchers at Wake Forest University School of Medicine has identified a promising strategy to treat brain metastases, one of the most challenging and deadly complications of lung cancer. The research team developed a highly specialized type of immune cell, called a CAR macrophage, or CARMA, designed to find and attack tumor cells that spread to the brain. These engineered macrophages were able to enter the brain, seek out cancer cells, and slow tumor growth in preclinical models.
The findings are published online in Nature Biomedical Engineering.
The Challenge of Brain Metastases
Brain metastases occur in nearly one in three patients with lung cancer, and current treatments, such as surgery and radiation, offer limited options because many drugs cannot cross the blood-brain barrier, the brain's natural defense system.
Engineering CARMA to Cross the Blood-Brain Barrier
The research team engineered macrophages to express a chimeric antigen receptor (CAR) that targets mesothelin, a protein found at high levels on lung cancer cells that have spread to the brain. To boost the macrophages' ability to activate and destroy cancer cells, the researchers added a signaling component called MyD88, which strengthens the cell's natural "attack" mode. The team then tested these MyD88‑CAR macrophages in several laboratory and mouse models designed to mimic lung cancer brain metastasis.
CAR macrophages successfully crossed the blood-brain barrier and accumulated in brain tumor regions. The MyD88‑enhanced version of CARMA showed stronger anti‑tumor activity than other tested versions. CARMA cells not only directly attacked tumor cells, but they also released helpful signals, including TNF‑α, that harmed nearby cancer cells even if those cells did not express the target antigen.
Treated models showed significant reductions in brain tumor progression and increased survival. CARMA showed fewer signs of toxicity in preclinical comparisons than CAR-T approaches tested in the study.
Future Clinical Testing
According to Watabe, most existing immunotherapies struggle to reach tumors inside the brain, and treatments that do reach the brain can sometimes cause severe side effects. However, this study demonstrates that engineered macrophages may offer a safer approach for patients whose cancer has spread to the brain.
The researchers will work to further refine the CARMA cell design and begin steps toward early-phase clinical testing. "Our ultimate goal is to translate this into a treatment option for patients," Watabe said. "There is a tremendous need, and we believe this technology has potential."