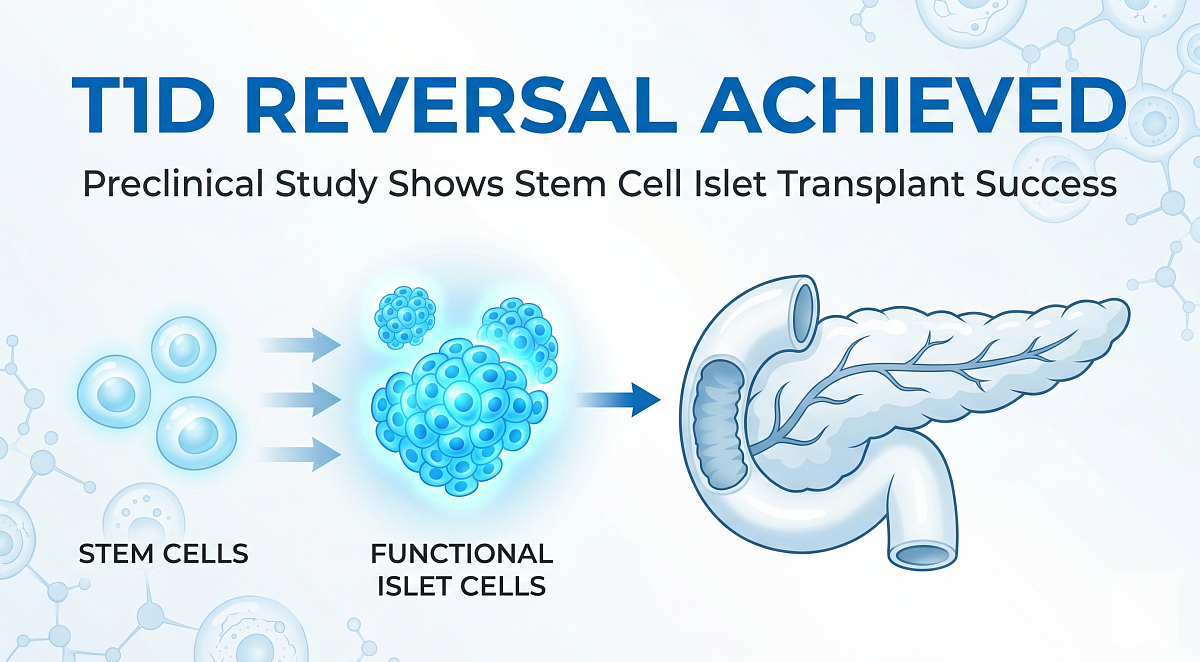
Researchers from Stanford Medicine have developed a novel transplant strategy that prevents and reverses Type 1 Diabetes in mice. By combining blood stem cell and pancreatic islet cell transplants from immunologically mismatched donors, they successfully halted autoimmune destruction of insulin-producing cells. Notably, the animals required neither insulin nor immunosuppressive drugs during the six-month study and showed no signs of graft-versus-host disease.
Creating a Hybrid Immune System
The team, led by Seung K. Kim, achieved this outcome by generating a hybrid immune system composed of both donor and recipient cells. This approach not only replaced lost islet cells but also reprogrammed the immune system to stop attacking them. Consequently, 19 out of 19 mice avoided developing diabetes, while 9 out of 9 mice with established disease were cured.
Reducing Radiation Exposure
In a follow-up study published in JCI Insight, researchers significantly reduced the radiation required before transplantation—from 225 centigray (cGy) to just 10 cGy. This advancement minimises risks such as infertility and cancer. As Stephan Ramos noted, lowering radiation doses makes the therapy safer and more accessible for broader patient populations.
Refining the Pre-Transplant Strategy
Building on earlier work, the team added immune-modulating drugs to improve transplant success in autoimmune conditions. Additionally, they used agents to clear bone marrow stem cells, enabling donor cells to engraft more effectively. As a result, treated mice remained disease-free, fertile, and free from complications.
Broader Implications for Autoimmune Diseases
As reported by medicalxpress, this research builds on foundational work by Samuel Strober and Judith Shizuru, who demonstrated long-term transplant tolerance using similar principles. Importantly, the new findings suggest potential applications beyond diabetes, including autoimmune disorders like Rheumatoid Arthritis and Lupus.
Path Toward Clinical Translation
Although challenges remain—such as sourcing sufficient islet cells—the researchers are exploring lab-grown alternatives and improved cell survival strategies. Ultimately, this approach could redefine treatment by safely resetting the immune system and enabling durable organ and cell replacement therapies.